 After reading a number of questions about acceptance into PA programs a prevailing theme has emerged.
After reading a number of questions about acceptance into PA programs a prevailing theme has emerged.
Many international physicians stated that their interest in becoming PAs stems from dissatisfaction with the hours or volume of patients they are seeing in their own practices in their native countries.
So, what is my advice?
That you make an honest, soul-searching assessment of what it is you are seeking.
PAs are Not an MD Surrogate
If you have a prevailing feeling that your MD is a superior credential and that you will be functioning as an "MD Surrogate" in the US, then perhaps you don't fully understand the concept of a PA/supervising MD team.
Every good PA knows very well our limits in the scope of practice which have served us and our physician mentors very well for over 40 years.
We aren't, and never will be physicians!
Nor will you, if you practice as a PA within your scope of practice.
PAs Don't Always Have Regular, Predictable Hours?
You may also want to investigate why you believe that coming to the United States to become a PA will ensure that your hours will be regular, predictable and better than what you have now.
Your hours will depend completely on the medical practice or hospital which hires you.
Expecting that as a PA you will have it easier than you have it as an MD may be a false assumption.
Many PAs work very long, grueling hours in emergency rooms, critical care, hospitals, public health facilities, family health care, community clinics and countless other fields in addition to volunteer work on their own time.
The person who inquired about coming to a US PA program because PAs in Canada are still new and not well respected might do well to step back for perspective.
R.E.S PA-C T
PAs in the US are the single most serially tested group of medical providers in the world.
We are currently changing a decades-old requirement for national board certification exams every six years to maintain our treasured "C" on our credential, indicating board certification.
But if you look closely at the environment which mandated our test schedule it reveals that we have been regularly asked to "prove" our knowledge, skills, and trustworthiness for those same decades.
Each of us went through some version of facing the "newness" question about what is a PA and scrutiny and occasional rejection by physicians, nurses, and patients.
And most of us will tell you the struggle to prove ourselves is hard.
And at one time it may have been necessary.
But now, for most situations, when you join a medical practice, your patients already know what a PA is and how we function with their physicians.
In Canada, your PA profession, though in comparative infancy to the US, needs great people to choose it, build its competence and support its growth rather than abandon it and go to already proven territory.
If you believe in rigorous academic and clinical training then wouldn't you want to be in the vanguard in Canada demanding that rigor?
The Good With the Challenging
I treasure my life and work as a PA in California and Florida.
Anyone fortunate enough to come here as an immigrant looking for an opportunity to serve in the medical corps is warmly welcomed and will be honored by our ranks.
But when you choose this path to PA make sure you are seeing the good with the challenging and accepting that part of being in medical care.
Every place in the world demands a near-total commitment of time and the humility to be comfortable caring for impoverished people, people of every cultural and ethnic background, just as you are doing wherever you currently live.
Your challenges are the same as ours in that regard.
The United States PA programs are unparalleled in preparing a workforce to address the overwhelming problem of inadequate access to health care.
But we may not be a panacea for overworked, over-scheduled and feeling unappreciated, at times.
Sincerely, and with good wishes for your success,
- Martie Lynch BS, PA-C
The Long Road to Practice
Today's post comes to us via the comments section and was written by physician assistant Margie Lynch, PA-C.
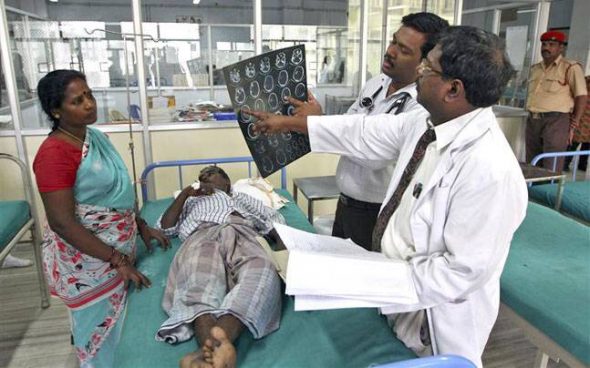
I receive many comments and emails from internationally trained doctors looking for career options here in the United States.
In fact, as an undergraduate, while working in the campus health clinic, I had the privilege of being trained by a foreign medical doctor from India who had transitioned to a laboratory tech in the United States.
The truth is, in many instances, a foreign medical degree is non-transferable and the barriers to practice prevent many highly skilled, well-intentioned international providers from coming to the United States. And like the MD I worked with, their skills and training may go to waste. This is a shame sad there are many clinics and hospitals in the US that would benefit from culturally competent bilingual practitioners.
And like the MD I worked with, their skills and training may go to waste. This is a shame sad there are many clinics and hospitals in the US that would benefit from culturally competent bilingual practitioners.
This is a shame as there are many clinics and hospitals in the US that would benefit from culturally competent, highly skilled, bilingual practitioners.
International Barriers to Practice in the United States
According to this NY Times Article, the United States already faces a shortage of physicians in many parts of the country, especially in specialties where foreign-trained physicians are most likely to practice, like primary care. And that shortage has gotten exponentially worse since the passage of the affordable healthcare act in 2014.
For years the United States has been training too few doctors to meet its own needs, in part because of industry-set limits on the number of medical school slots available. Today about one in four physicians practicing in the United States were trained abroad, a figure that includes a substantial number of American citizens who could not get into medical school at home and studied in places like the Caribbean.
But immigrant doctors, no matter how experienced and well trained, must run a long, costly and confusing gantlet before they can actually practice here.
The process usually starts with an application to a private nonprofit organization that verifies medical school transcripts and diplomas. Among other requirements, foreign doctors must prove they speak English; pass three separate steps of the United States Medical Licensing Examination; get American recommendation letters, usually obtained after volunteering or working in a hospital, clinic or research organization; and be permanent residents or receive a work visa (which often requires them to return to their home country after their training).
The biggest challenge is that an immigrant physician must win one of the coveted slots in America’s medical residency system, the step that seems to be the tightest bottleneck.
That residency, which typically involves grueling 80-hour workweeks, is required even if a doctor previously did a residency in a country with an advanced medical system, like Britain or Japan. The only exception is for doctors who did their residencies in Canada.
The whole process can consume upward of a decade — for those lucky few who make it through.
Fighting Brain Drain
The counterargument for making it easier for foreign physicians to practice in the United States — aside from concerns about quality controls — is that doing so will draw more physicians from poor countries. These places often have paid for their doctors’ medical training with public funds, on the assumption that those doctors will stay.
According to one study, about one in 10 doctors trained in India have left that country, and the figure is close to one in three for Ghana. (Many of those moved to Europe or other developed nations other than the United States.)
No one knows exactly how many immigrant doctors are in the United States and not practicing, but some other data points provide a clue. Each year the Educational Commission for Foreign Medical Graduates, a private nonprofit, clears about 8,000 immigrant doctors (not including the American citizens who go to medical school abroad) to apply for the national residency match system. Normally about 3,000 of them successfully match to a residency slot, mostly filling less desired residencies in community hospitals, unpopular locations and in less lucrative specialties like primary care.
In the United States, some foreign doctors work as waiters or taxi drivers while they try to work through the licensing process.
The International Path to PA
Is PA a reasonable alternative to foreign-trained medical providers whose skills we desperately need here in the United States?
And just how many PA schools are eagerly opening their doors to these practitioners?
This, my friends, is a topic for another blog post.
Feel free to share your thoughts in the comments section down below.
Warmly,
-Stephen Pasquini PA-C
Resources
Are you or someone you know a foreign trained doctor or a medical provider looking to practice as a PA in the US? Here are some useful resources:
- Here is a wonderful resource on the topic from the ARC-PA (they accredit US PA programs and determine who may sit for the PANCE exam)
- Physician Assistant Forum - Foreign medical graduate
- Dose of PA - From International Student to Physician Assistant
- NY Times Article - Path to United States Practice Is Long Slog to Foreign Doctors
















hello,
i am IMG from India. And I am green card holder of USA so,do i need to take TOFEL to apply for pa school? Can you send list of pa program which accept without TOFEL exam?
Hi Bhoomi, greetings from the USA! I created a PA school search site that allows you to filter by TOEFL requirements. Here is a list of the 55 programs in the USA that accept international students and don’t require the TOEFL: https://www.paschoolfinder.com/cat/toefl-not-required/
You can use the category search function or the program search and sort tool to filter this even further if you would like. Let me know if you have any more questions whatsoever!
Warmly,
Stephen Pasquini PA-C
http://www.smartypance.com
http://www.thepalife.com
Thanks for your reply.
I want to know, do you know any group of img work as pa, I want to be guided by previously experienced for my application.
Hi Bhoomi, I am sure if you search the internet, social media, FB, forums, etc you will be able to find a group… Or maybe it’s time to create one!! If you do please share that here and I can send people your way.
Stephen
Dear Stephen
Thank you very much for giving such a comprehensive information. More importantly I thank you for sympathising and empathetic approach to FMG. People’s need to migrate are very complex; no one leaves his comfort zone and family unless he has a compelling reason. They are not there to steal anyone’s meal, just trying to get a better meal for themselves….as humans have done for millenia. I thank you for not making the FMG’s belittled, which is what they feel reading other resources on the web.
Any chance PA schools offer some online courses, this could reduce the amount of time they have to spend in the actual premises. They can continue with their lives and study towards PA unless it is absolutely necessary to uproot themselves.
Hi AI, I appreciate your comment and sentiments! There is one fully online program that I am aware of, and that is the Yale PA program, although they only accept US residents. https://paonline.yale.edu/admissions/application-requirements/
I am sure more programs will start adopting some form of distance learning. If anything comes out of this whole COVID-19 pandemic, it may be an understanding of how to administer an online curriculum and the value/flexibility it offers to both faculty and students. We see the same adoption in the clinic setting, as well. For now, though, I think online courses for international students to attend US PA programs may be sadly non-existent.
Let me know if you find anything and I will be sure to share it.
Stephen Pasquini
Hi,
I’m a foreign trained dentist. What are the pre-requisites needed for me to pursue PA?
Holy Hell! WHAT HAVE READ HERE HAVE COMPLETELY BROKEN ME A PART FROM CONTINUING PURSUING MY CLINICAL MEDICINE AND COMMUNITY HEALTH IN AFRICA- YET I WAS HOPING OF FINISHING ABD GOIBGVTO US TO DO PANCE,THEN START PRACTICING…have realized have been building castles in the air.And the best thing to do is to cancel all am doing now here and go study my Medicine starting from any level accessible in US.Thanks all for your advice,it has helped from busting my ASS here for nothing doing medicine yet it won’t be recognized in US.
To all international medical graduates, this is a sane and personal advice. If you want to be a PA don’t even think of doing your USMLEs as it will be a total waste of time and precious money and a sure road to mental and monetary bankruptcy. Start a PA program as early as you can and then you are set for life as the trend in US is more towards mid-level practitioners than MDs or DOs. Remember that this country runs and survives on just one thing and that is money. Nowhere does money play such a big role as in this country. So if you want to achieve the “American Dream” be money minded and just see $$$ only. It is stupid to even think that a foreign medical graduate is not fit to sit for a PA exam but this has more to do with money than anything else. So it is all a game of money. PA programs need your money before you can make any.
Hi Paramjit, although I agree with many of your sentiments about American greed and money/corruption in the US medical system I don’t think PA program requirements of foreign medical graduates is simply a “money grab.” It’s important for the PA profession (and our patients’ safety) that we have professional standardization and US medical schools and US PA schools must meet strict regulatory requirements which may or may not comply with those of foreign institutions. I do think it’s disappointing that a well-trained foreign medical doctor must meet such barriers to continuing their profession in the US. From what I have heard it involves retaking boards and completing residency training again in the US, which is not easy. It’s also quite difficult for a foreign trained MD to apply and be accepted into PA school in the US without appearing as though they are just “settling.” To better serve our patients it might be time to create less friction so that we can make sure well trained and highly qualified foreign graduates can put their hard work and skill to good use. It’s a shame otherwise.
Stephen
GREETINGS.
PLEASE SIR, HTIS IS MY CURRICULUM .
I M PHYSICIAN FROM MOROCCO.
BORN IN MOROCCO IN 11/28/1964.
I M GRADUATE FROM UNIVERSITY OF MEDICINE OF
RABAT IN 1995.
I WORKED
WITH MINISTRY OF HEALHT OF MOROCCO SINCE 1998.
I HAVE ONE YEAR OF EXPERIENCE
IN NUCLEAR MEDICINE IN SWITZERLANDN ,SUISSE. LAUZANE ,
WITHE THAOUSAND 1000 OF CASES
OF SCINTIGRAPHIE OF BONE AND THYROIDE DISEAS
2003.
I HAVE LOT OF RESEARCHES IN EPIDEMEOLOGY IN
2014 THAT S CAN VERY INTERSTE FOR
YOUR UNIVERSITY
I HOLD VISA TOURIST B1/B2.
I WANT TO TRAVEL TO USA IN
ORDER TO
LOOKING FOR
INSCRIPTION AND TO BEGAN WITH YOU AS PA .
PLEASE TEL ME ABOUT FIRST STEP
CAN I DO.
Good day my name is peter markus de jesus practicing in general pediatrics here in the philippines for 6 years now, im a greencard holder in the USA , and plan to take a path as a Physician Assistant, can you help me what steps and requirement do i need to prepare to accomplish , Thanks for the help and Godbless
Dear Stephen,
I am an IMG from India practicing dermatology in India since 5 years .My Gre score is 298,AWA -3 ,IELTS -7 .I would like to join the PA program in USA and continue as a dermatology PA
.Which schools are best to join ,Can I apply for the PA program 2019.
Thank you
Hi Meena,
From the standpoint of the ARC-PA, individuals educated as physicians outside of the United States are not treated any differently than any other prospective PA student. To practice as a PA in the United States one must graduate from an ARC-PA accredited program and be certified by the NCCPA. If interested in applying to a PA program, such individuals should contact the PAEA for information on specific programs.
Here is a wonderful resource on the topic from the ARC-PA (they accredit US PA programs and determine who may sit for the PANCE exam): http://www.arc-pa.org/frequently-asked-questions/non-us-health-care-professionals/
Before you can work in the US, you must contact the Commission on Graduates of Foreign Nursing Schools (CGFNS International) to complete a visa screening program which, in part, will determine if your education was equivalent to that from a US PA Program. If your education is equivalent, you are eligible for a certificate that you can submit with your visa application to the US State Department. The State Department’s approval of your occupational visa may help you enter the U.S. but you are still not eligible to work as a PA in the U.S.
To become a PA in the United States, individuals must also attend and graduate from an ARC-PA–accredited entry-level PA program and pass the Physician Assistant National Certifying Exam (PANCE) administered by the National Commission on Certifying of Physician Assistants (NCCPA).
For information on PA programs contact the Physician Assistant Education Association (PAEA): https://paeaonline.org/ and the directory of PA programs here: http://directory.paeaonline.org/
Eligibility criteria for taking the Physician Assistant National Certifying Exam (PANCE) are available on the NCCPA web site: http://www.nccpa.net/
Additional information on practicing as a PA in the US can be found at the American Academy of Physician Assistants’ (AAPA) website: https://www.aapa.org/
To determine if an individual state allows non-US educated physicians to practice as PAs without additional education and national certification, you would have to contact the licensing bodies of the specific states.
To find PA programs that accept International students:
I would start by searching the PAEA directory website and click the box “Accept int’l applicants.” Currently, there are 138 programs that accept international students. From there you need to narrow down further based on requirements. I would then use my PA program picker table. You can narrow your search even further using all your variables: https://www.thepalife.com/pa-program-picker/
Then, follow the links to the PA program websites and reach out to them personally. They will be able to guide you better than I since every program is a bit different. If you have any questions afterward just shoot me a reply.
Stephen
Hi, i’m a interne in haiti about to get graduate from medical school in a few months, i was wondering if i have a chance to Be accepted in the program as PA?
Hi Reynaud,
Here is a response I just left for another applicant I think it applies to your situation as well:
From the standpoint of the ARC-PA, individuals educated as physicians outside of the United States are not treated any differently than any other prospective PA student. To practice as a PA in the United States one must graduate from an ARC-PA accredited program and be certified by the NCCPA. If interested in applying to a PA program, such individuals should contact the PAEA for information on specific programs.
Here is a wonderful resource on the topic from the ARC-PA (they accredit US PA programs and determine who may sit for the PANCE exam): http://www.arc-pa.org/frequently-asked-questions/non-us-health-care-professionals/
Before you can work in the US, you must contact the Commission on Graduates of Foreign Nursing Schools (CGFNS International) to complete a visa screening program which, in part, will determine if your education was equivalent to that from a US PA Program. If your education is equivalent, you are eligible for a certificate that you can submit with your visa application to the US State Department. The State Department’s approval of your occupational visa may help you enter the U.S. but you are still not eligible to work as a PA in the U.S.
To become a PA in the United States, individuals must also attend and graduate from an ARC-PA–accredited entry-level PA program and pass the Physician Assistant National Certifying Exam (PANCE) administered by the National Commission on Certifying of Physician Assistants (NCCPA).
For information on PA programs contact the Physician Assistant Education Association (PAEA): https://paeaonline.org/ and the directory of PA programs here: http://directory.paeaonline.org/
Eligibility criteria for taking the Physician Assistant National Certifying Exam (PANCE) are available on the NCCPA web site: http://www.nccpa.net/
Additional information on practicing as a PA in the US can be found at the American Academy of Physician Assistants’ (AAPA) website: https://www.aapa.org/
To determine if an individual state allows non-US educated physicians to practice as PAs without additional education and national certification, you would have to contact the licensing bodies of the specific states.
To find PA programs that accept International students:
I would start by searching the PAEA directory website and click the box “Accept int’l applicants.” Currently, there are 138 programs that accept international students. From there you need to narrow down further based on requirements. I would then use my PA program picker table. You can narrow your search even further using all your variables: https://www.thepalife.com/pa-program-picker/
Then, follow the links to the PA program websites and reach out to them personally. They will be able to guide you better than I since every program is a bit different. If you have any questions afterward just shoot me a reply.
Stephen
Hello Reynaud, I am from Haiti too, I need more information can you call me 9084042719 or email me : [email protected]
I graduate from faculty of dentistry elmini university egypt
Hi Mohamed,
Here is a wonderful resource on the topic from the ARC-PA (they accredit US PA programs and determine who may sit for the PANCE exam) on the topic: http://www.arc-pa.org/frequently-asked-questions/non-us-health-care-professionals/
Before you can work in the US, you must contact the Commission on Graduates of Foreign Nursing Schools (CGFNS International) to complete a visa screening program which, in part, will determine if your education was equivalent to that from a US PA Program. If your education is equivalent, you are eligible for a certificate that you can submit with your visa application to the US State Department. The State Department’s approval of your occupational visa may help you enter the U.S. but you are still not eligible to work as a PA in the U.S.
To become a PA in the United States, individuals must also attend and graduate from an ARC-PA–accredited entry-level PA program and pass the Physician Assistant National Certifying Exam (PANCE) administered by the National Commission on Certifying of Physician Assistants (NCCPA).
For information on PA programs contact the Physician Assistant Education Association (PAEA): https://paeaonline.org/ and the directory of PA programs here: http://directory.paeaonline.org/
Eligibility criteria for taking the Physician Assistant National Certifying Exam (PANCE) are available on the NCCPA web site: http://www.nccpa.net/
Additional information on practicing as a PA in the US can be found at the American Academy of Physician Assistants’ (AAPA) website: https://www.aapa.org/
To determine if an individual state allows non-US educated physicians to practice as PAs without additional education and national certification, you would have to contact the licensing bodies of the specific states.
Stephen
Dear Stephen,
Is it for a Canadian PA to work in the US?
Thank you,
Naomi
H, Naomi here is a great thread on this exact topic on the physician assistant forum: https://www.physicianassistantforum.com/topic/942-can-canadian-pas-practice-in-usa/
The short answer is, to work as a PA in the US you have to pass the PANCE and in order to take the PANCE, you must have graduated from a program that the NCCPA deems accredited.
So, either
1) the NCCPA must recognize the accreditation process in Canada as equivalent to the one in the USA (In Canada it’s CAPA: http://www.caopa.net/ btw)
or
2) They must change the policy slightly
Stephen